
The pathway is composed of the dorsal column within the spinal cord and the medial lemniscus in the brain stem. From here, the signal travels through the dorsal column–medial lemniscus pathway. The intensity of the vibration must cause the neuron(s) to reach or surpass a threshold in order for an action potential to be propagated. 
The outside stimulus is a vibration that activates one of the three encapsulated nerve endings based upon where the sensation is felt. The sensory conduction pathway that allows for cognitive recognition of vibration occurs through afferent neurons, also known as sensory neurons. Pathway The image on the left side depicts the dorsal column pathway for vibration perception. Merkel disk receptors and tactile corpuscles respond best to low frequencies when producing an action potential. The Merkel disk receptors are located in the superficial epidermis and in hair follicles, while tactile corpuscles are concentrated heavily in the fingertips. The Pacinian corpuscles are located within the deeper layer of the skin, under the skin in the subcutaneous tissues, within muscles, in the periosteum, and other deeper layers of the body. Pacinian corpuscles, Merkel disk receptors, and tactile corpuscles are all encapsulated nerve endings involved in tactile stimulation. Receptors The second neuron in the figure depicts an encapsulated nerve ending. This works because bones are good resonators of vibrations. To determine whether a patient has diminished or absent pallesthesia, testing can be conducted using a tuning fork at 128 Hz by placing it on the skin overlying a bone. Damage to the peripheral nervous system or central nervous system can result in a decline or loss of pallesthesia.Ī diminished sense of vibration is known as pallhypesthesia. The afferent neuron travels to the spinal column and then to the brain where the information is processed. All of these receptors stimulate an action potential in afferent nerves (sensory neurons) found in various layers of the skin and body. This sensation, often conducted through skin and bone, is usually generated by mechanoreceptors such as Pacinian corpuscles, Merkel disk receptors, and tactile corpuscles. A tuning fork is a useful screening test for diabetic neuropathy.Pallesthesia (\ˌpal-es-ˈthē-zh(ē-)ə\), or vibratory sensation, is the ability to perceive vibration. The tuning fork reliably detected peripheral neuropathy in comparison with the neurothesiometer. The plot of the difference of both methods against their mean yielded a good agreement of the two VPT measurements, and the tuning fork had a high sensitivity and positive predictive value for the diagnosis of abnormal bedside tests and for symptomatic neuropathy. 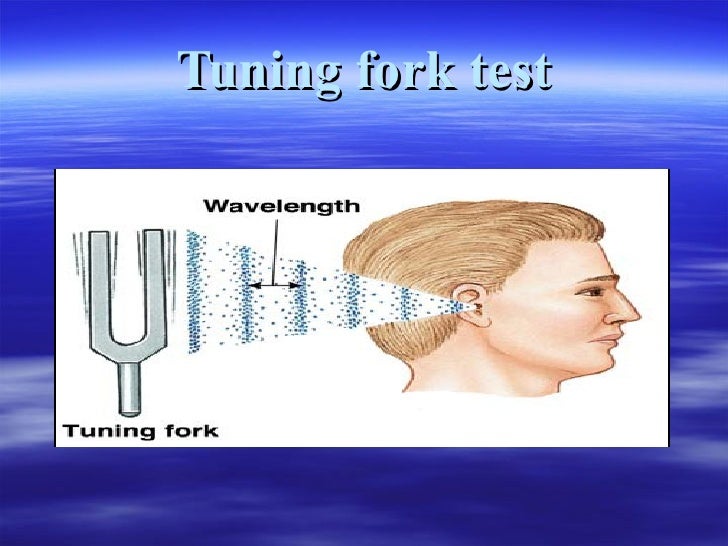
Finally, the VPT measured by the neurothesiometer was 2.5 times higher in patients with an abnormal tuning fork test (32.0 +/- 9.8 vs. The same was true for the percentages of an abnormal 10-g monofilament test (66.7% vs. Patients with an abnormal vibration test were significantly (P < 0.0001) older than subjects with a normal vibration sense, while diabetes duration and HbA(1c) of the former were also significantly elevated. VPT was normal in 1917 subjects and abnormal in 105 (5.2%) patients when measured by the tuning fork. VPT was also measured in 175 non-diabetic control subjects to define normal values. These evaluations were further combined to diagnose peripheral nerve dysfunction (abnormal bedside tests) and symptomatic neuropathy. In 2022 consecutive diabetic subjects, peripheral polyneuropathy was diagnosed by vibration perception threshold (VPT) at the tip of both great toes using a 128-Hz tuning fork and a neurothesiometer, by simple bedside tests and by the presence of neuropathic symptoms. 
The aim of the study was to investigate the predictive value of the Rydel-Seiffer tuning fork for detecting diabetic neuropathy and to compare it with an electronic neurothesiometer.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
